Open claims and closed payer claims data are essential for understanding the status and activities of patients along their healthcare journey, but which data type is most useful and when? Whether the intent is to measure the cost effectiveness of a newly launched drug or to optimize clinical trial recruitment, both open claims data and closed payer claims data provide unique benefits that make each suitable for different types of research by life sciences companies.
- Open claims data is derived from broad-based healthcare sources and can highlight a patient’s activities over a longer timeframe, regardless of a patient’s insurance provider.
- Closed payer claims data is derived from health insurance providers (payers), revealing nearly all of a patient’s healthcare activities during a specific enrollment period.
- Platforms like taXonomy make it easy to access open claims or closed payer claims that reveal a patient health journey.

What are open claims?
Open claims data includes both medical claims and pharmacy claims primarily sourced from clearinghouses, pharmacies and software platforms. Other open data types, or those not sourced from insurance providers, include lab results and electronic medical records (EMR).
Open medical claims can be captured in a few ways:
- When a patient goes to the doctor, the visit may be recorded in the practice management system (PMS), the EMR and the billing system.
- Data is also captured when the doctor transmits the medical claim (837, the bill sent to the payer) through a clearinghouse or switch to the appropriate insurance provider.
- After the doctor submits a requested reimbursement amount, the insurance provider decides what will actually be paid, which is captured in a remittance (835, the payment decision sent back to the provider).
Open pharmacy claims also originate from a variety of sources:
- When a patient receives a prescription, their doctor will record it in the EMR.
- When the prescription is transmitted to the pharmacy, that will be captured in the pharmacy management system and by the pharmacy benefits manager (PBM).
- After the insurance provider authorizes and adjudicates the claim, it could also pass through another clearinghouse or switch when the patient receives their medication.
Main sources for open claims data
Since open claims encompass multiple data types, they offer insights into patient touch points across the healthcare landscape with no limitations on time frame. The recency of this data is a key differentiator. The table below lists where open claims data originates from the medical and pharmacy side.
 MEDICAL
MEDICAL
|
 PHARMACY
PHARMACY
|
|---|---|
| → Practice management system (PMS) | → Electronic prescription |
| → Electronic medical record (EMR) | → Electronic medical record (EMR) |
| → Billing system | → Pharmacy benefits manager (PBM) |
| → Clearinghouse or switch | → Clearinghouse or switch |
Many medical, pharmacy and lab visits within the open claims data can be seen as recently as yesterday, offering near-real-time reporting and tracking. Standard data fields, such as ICD-10 codes and CPT codes, are available in addition to submitted and paid cost information, physician information, referring NPI, place of service and more.
Life sciences can utilize open claims data to power clinical trial optimization, regulatory and safety measures, health economics and outcomes research (HEOR), value-based agreements, data governance, marketing campaigns, and much more.
Open claims in practice
Patient X is currently seeing four different doctors for a multitude of medical issues. Data from three of those doctors: a primary care physician, an endocrinologist and an ENT, are captured within the available open claims dataset. As long as the patient continues to see the same doctors (who use the same clearinghouses), open claims will capture the relevant data, regardless of their insurance provider.
The fourth doctor Patient X is seeing, a cardiologist, uses a different clearinghouse than the three others. Because that clearinghouse is not included in the open claims dataset, the visit to this doctor may never be “seen” in the data. Gaps in a patient journey are common when using open claims data because it is often difficult to know what percentage of interactions are captured. Appending the journey with additional insights from other datasets, such as lab and EMR data, can help piece together a more comprehensive view.
What are closed payer claims?
Closed payer claims data is derived from the insurance provider (or payer) and captures nearly all events that occur during a patient’s enrollment period, including medical and pharmacy visits and transactions for both retail and specialty settings. This reveals a valuable look into the patient journey and connects patients’ diagnoses, actions and decisions along the way with minimal gaps. A platform like taXonomy is a comprehensive resource of open and closed payer claims.
Main sources for closed payer claims
Closed payer claims coverage is available for nearly all interactions a patient has within the healthcare system. This includes ICD-10 codes, CPT codes, physician and specialty information, geographic information, as well as nearly all medical and pharmacy claims.
Closed payer claims data includes commercial, Medicare and Medicaid plans with an average lag time of 90 days, typically much longer than that of open claims data. Overall, the information from insurance carriers offers a more comprehensive patient journey during their enrollment period.
The main source for closer payer claims is always the insurance carrier:
Medical claims from the insurance carrier Pharmacy claims from the insurance carrier
Closed payer claims in practice
While it is possible to see a comprehensive view of a patient’s actions through closed payer claims, the average person in the U.S. changes their insurance provider fairly regularly. For example, Patient X may have been with their employer for the past three years and covered under its employer-provided health plan (Insurance provider A). If this specific provider is included within the closed payer claims dataset, nearly all of Patient X’s healthcare interactions will be captured during their enrollment period.
Once Patient X moves to another employer, it is very likely that the new company will offer a different plan from a different health insurance provider (Insurance provider B). So although nearly all interactions across all healthcare settings are captured for those three years, the patient may no longer be visible in this closed payer claims dataset.
Closed payer claims display a comprehensive view across all healthcare settings, but only for the enrollment period included in the dataset. Open claims data tends to provide a glimpse into the patient journey across several data sources over an open-ended time period.
How to create a comprehensive patient journey
Consider the following patient journeys as seen through open claims and closed payer claims data. Patients move through the healthcare ecosystem and open and closed claims data is collected:
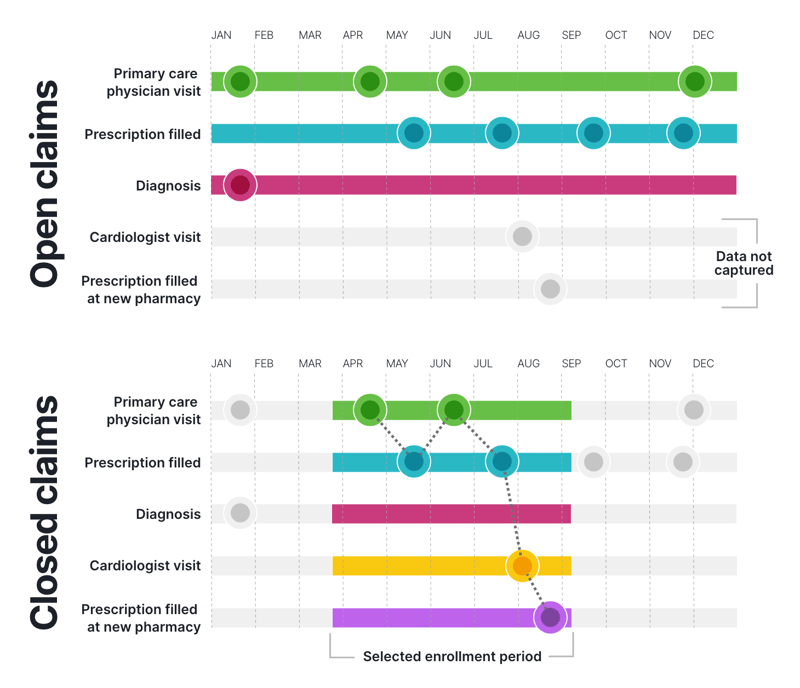
By combining both data types, researchers gain a more complete and accurate view of the patient journey. A tool that helps you do this is the HealthVerity taXonomy platforms, which offer synchronized access to both open and closed claims, delivering deeper insights and enhanced accuracy for real-world evidence generation.
If you want to explore patient counts and overlaps in real time, HealthVerity Marketplace is a one-stop platform where you can get real-world data that’s accurately synced, HIPAA privacy-compliant, and ready to use.
Closed and open claims use case: Chronic Obstructive Pulmonary Disease (COPD)
When studying a disease such as COPD, building context around the patient and their healthcare journey is crucial. Both open claims and closed payer claims are incredibly useful in studying the relevant behaviors of these patients, each with their own unique advantages.
Open claims
Since open claims data contains information from a variety of healthcare settings and doesn't rely on a patient maintaining the same insurance plan, the patient can be studied over a longer period of time. Open claims can indicate when the patient was diagnosed with COPD, what treatments they have received and if they have been referred to another doctor. EMR data may also provide the patient’s FEV1/FEC ratio, which can indicate whether the patient’s lungs are actually improving or worsening, providing a clearer picture of the patient's health.
Closed payer claims
Closed payer claims are equally useful for studying a more complete patient journey related to COPD. With closed payer claims, researchers can be confident about a patient’s adherence to treatment. They can also be certain if a patient is hospitalized for COPD or for other illnesses unrelated to their COPD diagnosis. This data will capture nearly all actions a patient takes during the window of enrollment, including those related to COPD and those that aren’t.
Open claims + closed payer claims
Combine open data types, such as lab and EMR, with closed payer claims to explore actions and treatments before, during and after a COPD patient is enrolled with a specific insurance provider. A longer history of the patient leading up to the diagnosis plus a comprehensive view of actions during enrollment adds valuable context to patient behaviors, diagnoses, treatments and adherence.
Open claims and closed payer claims are crucial for patient-centric research. Open claims are best for longitudinal studies and have specific fields that closed payer claims do not, such as referring physician. While open claims data provides a sampling of the journey over a long period of time, closed payer claims data offer a clear snapshot of activity covering nearly all activities during a set time frame. Both types can be used across many areas of outcomes research, with even more power when combined.
Looking to power your real-world evidence research with synchronized real-world data, including open and closed claims? Request a demo below or get in touch with our team.







